[HGPI Policy Column] (No.70) — From the Planetary Health Project “Part 17: The Lancet Countdown: A ‘Lifeline’ for Health and Economy Brought about by Climate Action”
date : 4/15/2026
![[HGPI Policy Column] (No.70) — From the Planetary Health Project “Part 17: The Lancet Countdown: A ‘Lifeline’ for Health and Economy Brought about by Climate Action”](https://hgpi.org/en/wp-content/uploads/sites/2/HGPI_20260410_Lancet-Countdown-Column.png)
<POINTS>
- The 2025 report of the Lancet Countdown on health and climate change: “Climate change action offers a lifeline” has been published. The report, published annually in The Lancet, tracks the world’s response to climate change and the resulting health benefits and costs.
- 2024 was the first year where average annual temperatures were 1.5°C above pre-industrial levels, with 12 out of 20 health risk indicators reaching record high levels. Under the current policy, the temperature is expected to rise by 2.7°C by 2100. Heatwave exposure hit a record high of 48.5 days per person in Japan, of which 28.8 days would not have occurred without anthropogenic climate change.
- Labor productivity is going down due to extreme heat. Japan lost 1.42 billion potential labor hours in 2024, representing a massive $49.42 billion in potential income loss, roughly 1% of Japan’s GDP. Heat-related deaths in Japan have increased by 136% compared to the 1990s.
- Japan allocated $70.27 billion on fossil fuel subsidies in 2023. By prioritizing these subsidies as public health costs rise, the government is effectively funding the environmental hazards that destabilize the healthcare system, and contributing to approximately 81,000 annual deaths in Japan due to PM2.5 air pollution.
Introduction
The relationship between human health and the environment has reached a point of severe tension. Since its inception in 2016, the Lancet Countdown on Health and Climate Change has served as the world’s most comprehensive monitoring system for this relationship. What distinguishes the 2025 Report, published ahead of COP30 in Belém, Brazil and intended to provide evidence base for the Nationally Determined Contributions (NCDs) and the Belém Action Plan, is its tone of extreme urgency. It frames climate action not as an optional green initiative, but as a lifeline to prevent the collapse of global health systems.
Understanding the data provided by the Lancet Countdown is essential. It provides the evidence base needed to move beyond abstract environmentalism and toward concrete, health-centered policy reform.
The Lancet Countdown: Project Transition and Current Status
The Lancet Countdown: Tracking Progress on Health and Climate Change is an international research collaboration headquartered at University College London (UCL) and funded by the Wellcome Trust. It was established following the 2015 Lancet Commission on Health and Climate Change, which reached two landmark conclusions: that unmitigated climate change would threaten to undermine fifty years of hard-won gains in global public health, and that a robust response to climate change could represent the greatest global health opportunity of the twenty-first century. Building on these findings, the “Countdown to 2030” was formally launched in 2016 with the explicit mandate to report annually the world’s response the climate change and the health benefits or costs in The Lancet from 2016 to 2030, the deadline for achieving the Paris Agreement’s most ambitious temperature targets.
The 2016 report was a prototype, establishing five thematic domains (Figure 1). Over successive editions, the indicator set has grown substantially. The 2025 report tracks 57 indicators, compared to 40 in the inaugural edition (Figure 2). Each year’s findings are published ahead of the UN climate negotiations, positioning the Countdown as an important source of evidence for global climate diplomacy. Moreover, the project matured into an annual publication in The Lancet, supported by over 300 researchers and UN agencies. It became the “Gold Standard” for climate-health data.
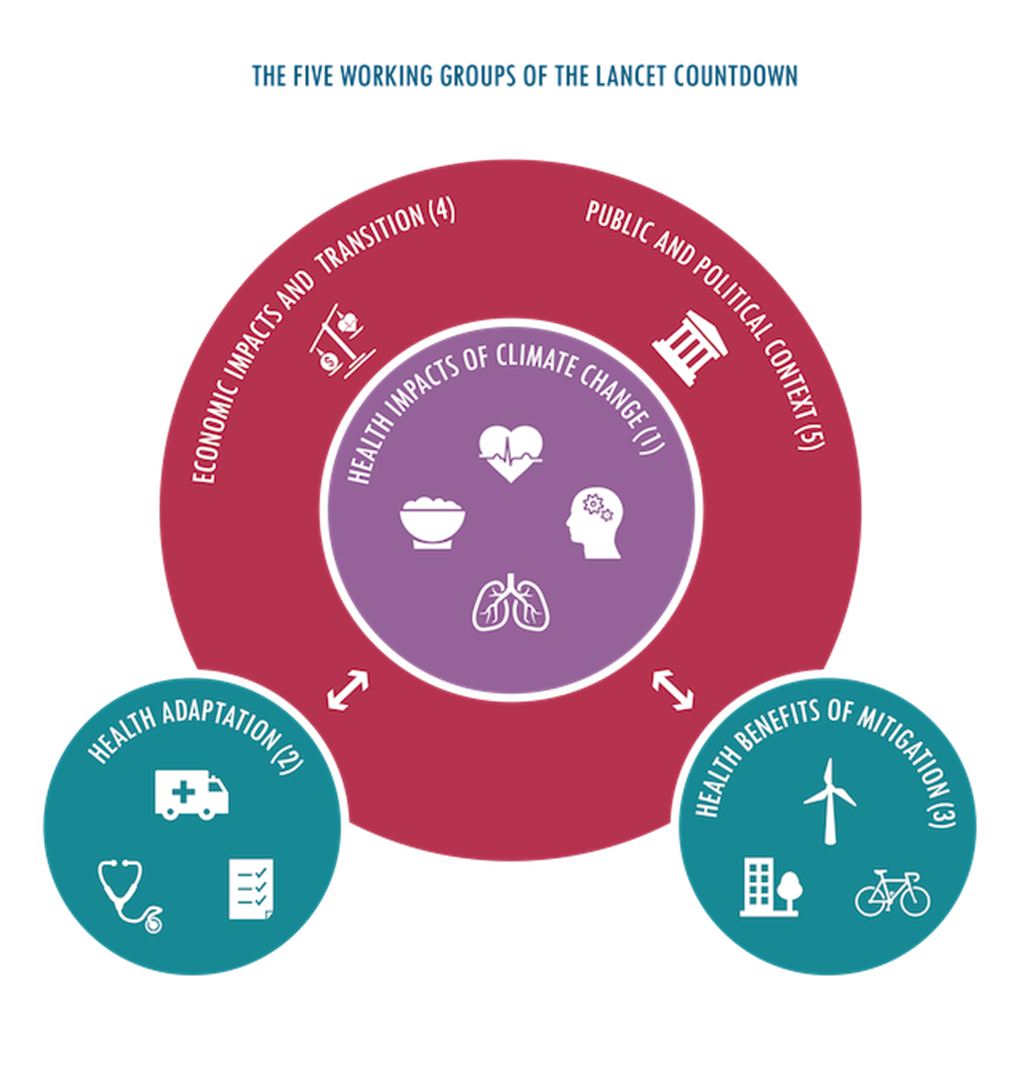
Figure 1: The five thematic domains of the Lancet Countdown
Source: The Lancet Countdown. Explore our data. https://lancetcountdown.org/explore-our-data/ (Accessed: 20 March 2026). License: CC BY-NC-SA 4.0
|
1: Health hazards, exposure, and impacts 1.1: Heat and health 1.1.1: Exposure of vulnerable populations to heatwaves 1.2: Extreme weather-related events and health 1.2.1: Wildfires 1.3: Climate suitability for infectious disease transmission 1.3.1: Dengue 1.4: Food security and undernutrition |
2: Adaptation, planning, and resilience for health 2.1: Assessment and planning of health adaptation 2.1.1: National assessments of climate change impacts, vulnerability, and adaptation for health 2.2: Enabling conditions, adaptation delivery, and implementation 2.2.1: Climate information for health 2.3: Vulnerabilities, health risk, and resilience to climate change 2.3.1: Vulnerability to severe mosquito-borne disease |
|
3: Mitigation actions and health co-benefits 3.1: Energy use, energy generation, and health 3.1.1: Energy systems and health 3.2: Air quality and health co-benefits 3.2.1: Mortality from ambient air pollution by sector 3.3: Food, agriculture, and health co-benefits 3.3.1: Emissions from agricultural production and consumption 3.4: Tree cover loss 3.5: Health-care sector emissions and harms |
4: Economics and finance 4·1: The economic impact of climate change and its mitigation 4.1.1: Economic losses due to weather-related extreme events 4.2: The transition to net zero-carbon, health-supporting economies 4.2.1: Employment in low-carbon and high-carbon industries 4.3: Financial transitions for a healthy future 4.3.1: Clean energy investment |
|
5: Public and political engagement with health and climate change 5.1: Media engagement 5.2: Individual engagement 5.3: Scientific engagement 5.3.1: Scientific articles on health and climate 5.4: Political engagement 5.4.1: Government engagement 5.5: Corporate sector engagement |
Figure 2: The indicators of the 2025 report of the Lancet Countdown on health and climate change
Source: Adapted from Romanello et al. (2025)
A critical evolution in the Countdown’s organizational architecture has been the progressive development of Regional Centres (Figure 3). These centres were established to ensure that globally aggregated findings are complemented by locally rooted analysis capable of informing the specific policy contexts of different regions. The establishment of these centres was also an important moment for Japan, with the launch of the Lancet Countdown Asia Center at Tsinghua University in 2020. This allowed for downscaled data, moving from global averages to country-level data sheets. This regionalization is critical because climate risks in a highly urbanized, aging society like Japan differ greatly from those in the Global South.
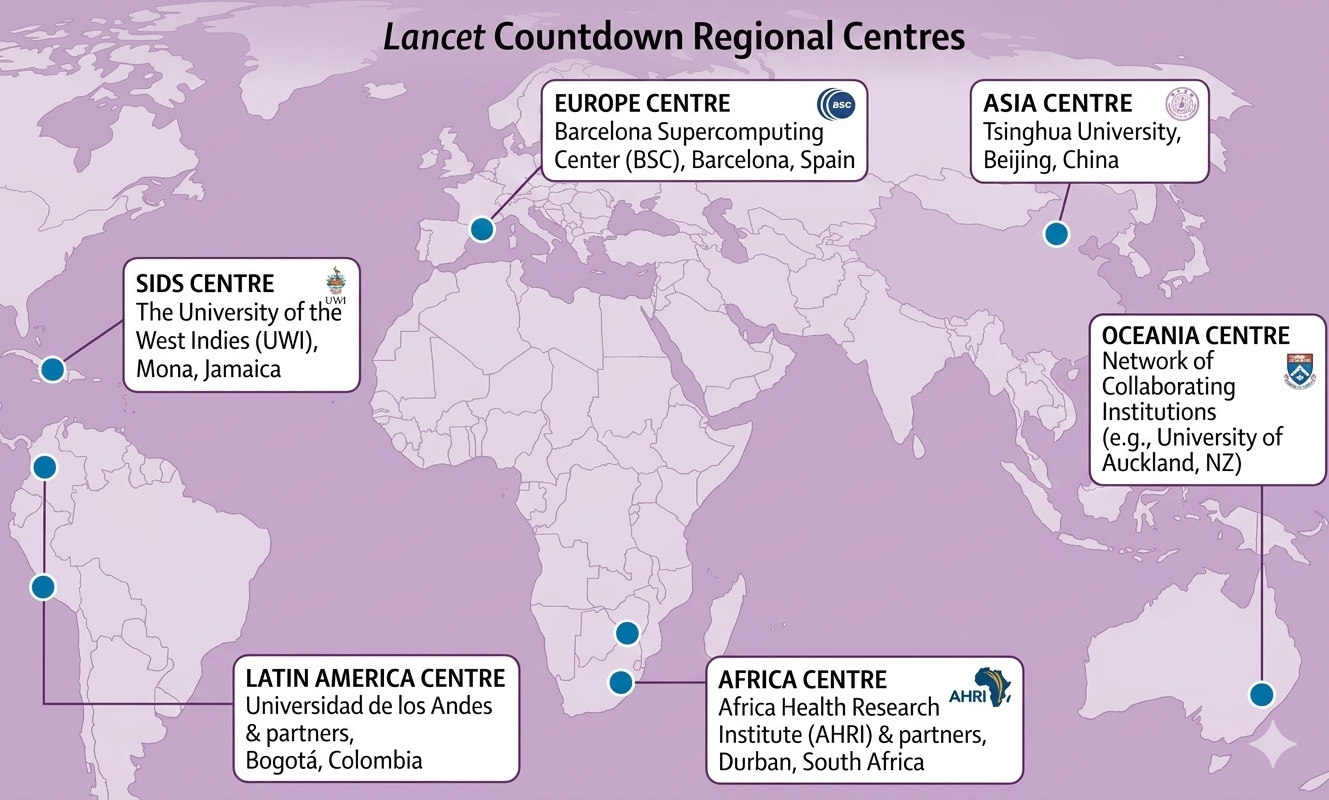
Figure 3: The Lancet Countdown’s Regional Centres
Source: Based on data from the Lancet Countdown (n.d.)
Global Health Hazards and Impacts
The 2025 Global Report presents an alarming outlook. Global greenhouse gas emissions reached record levels in 2024, and the resulting health hazards are now outpacing our capacity to adapt.
- Heat and Mortality: Globally, heat-related deaths increased by 23% compared to the 1990s, now averaging approximately 546,000 deaths annually. Between 2020 and 2024, 84% of all heatwave days that populations experienced would not have occurred in the absence of human-caused climate change. Moreover, in 2024 alone, 640 billion potential working hours were lost globally due to heat. This translated to potential income losses of $1.09 trillion, with 75.5% of labor losses in low HDI countries concentrated in agriculture, meaning that these losses are profoundly inequitable.
- Infectious Diseases: Climate change is also reshaping the landscape of infectious disease transmission. The transmission potential for dengue fever, already responsible for 7.6 million reported cases globally in early 2024, has increased by up to 49% since the 1950s. Leishmaniasis risk has grown by 29.6% and 364 million additional people are now at risk from tick-borne diseases compared to the 1950s. A record 91,195 kilometers of coastline were identified as suitable for Vibrio bacterial transmission in 2024, driven by warming sea surface temperatures.
- The Food Crisis: Food security represents a critical dimension of the health crisis. The 2025 report estimates that higher heatwave exposure and increased drought months in 2023 were associated with 123.7 million more people experiencing moderate or severe food insecurity across 124 countries.
Latest Analysis and Priorities for Japan
The Lancet Countdown’s 2025 data sheet for Japan shows a comprehensive overview of a high-income country navigating the intersection of rapidly escalating climate health risks, structural energy policy challenges, and a rapidly aging population.
Japan’s demographic profile makes it exceptionally vulnerable to extreme heat. Between 2012 and 2021, Japan saw an average of 4,300 heat-attributable deaths annually, a 136% increase from the 1990s. In 2024, the average person in Japan was exposed to 48.5 heatwave days. Crucially, the Lancet Countdown notes that 28.8 of those days would not have happened without anthropogenic climate change. Moreover, in 2024, Japan lost 1.42 billion potential labor hours due to heat, which represents $49.42 billion in lost economic potential. The service sector was hardest hit (33% of losses), followed by manufacturing (24%).
Japan’s extensive coastline and dense coastal populations create a second tier of climate health risk that extends beyond heat. Approximately 6.59 million people live in areas less than one meter above sea level, a population being acutely vulnerable to the combination of sea level rise, storm surge intensification, and coastal flooding. Coastal sea surface temperatures are already 1.72°C higher than the 1981–2010 average, threatening marine ecosystems that underpin food security and traditional livelihoods in fishing communities. Moreover, rising seas don’t just cause floods, they contaminate water supplies and increase the risk of waterborne diseases in densely populated coastal cities like Tokyo and Osaka. They also cause erosion of coastal infrastructure including healthcare facilities, and force communities to relocate. These events can also have lasting mental health and social impacts.
The Lancet Countdown data also present a challenging picture of Japan’s energy profile. Japan continues to rely heavily on coal, which accounts for 28% of total energy supply and 29% of electricity generation. Meanwhile, renewable energy accounts for just 3% of total energy supply, among the lowest in any high-income country. This structural fossil fuel dependence has direct health consequences: 81,200 deaths from anthropogenic outdoor PM2.5 air pollution were recorded in Japan in 2022, including 7,800 deaths attributable to coal combustion and 12,600 to transport sector emissions. Furthermore, in 2023, Japan spent $70.27 billion on fossil fuel subsidies, generating a net-negative carbon revenue balance in which subsidy expenditure exceeds revenues from carbon pricing.
Diet and food systems are another important part of the climate and health relationship in Japan. Red meat and dairy consumption account for about 29% of emissions from Japan’s agricultural consumption. At the same time, emissions linked to these foods have declined by 27% since 2000, indicating some progress. Diet also has major implications for public health. The 2025 data estimate that around 194,400 deaths in Japan are associated with insufficient consumption of nutritious plant-based foods such as fruits, vegetables, legumes, whole grains, nuts, and seeds. In addition, about 11,900 deaths are linked to high consumption of dairy, red meat, and processed meat.
Discussion: Toward Health-Centered Climate Policy
Drawing on the evidence presented by the Lancet Countdown, four major priority areas can be identified that are relevant to Japan’s climate governance as well as its internationalcommitments.
- Heat Action Planning for an Aging Population
Japan faces a unique challenge: rising heat exposure combined with one of the world’s most rapidly aging populations. This combination makes heat a particularly serious public health risk.
The mortality and labor data mentioned before indicate that current adaptation measures have not kept pace with rapidly accelerating heat risks. Addressing this will require a coordinated national strategy spanning health services, urban planning, labor policy, and social care. Key measures could include expanding access to cooling centers, providing financial assistance for cooling in low-income elderly households, strengthening workplace protections for heat exposure, and increasing investment in urban greening and heat-resilient infrastructure. Early warning systems and stronger health monitoring can also help protect vulnerable populations, particularly elderly individuals who live alone or have limited social support. Considerations should also be given to equity in access to cooling within Japan, especially for lower-income households and communities facing regional disparities in infrastructure and services.
- Coastal Adaptation and Health Resilience
Japan has many years of experience in coastal engineering and flood protection. However, the health impacts of coastal climate risks have not always been fully considered. Japan’s Climate Change Adaptation Act, adopted in 2018, established a national climate impact assessment that is updated every five years. This framework provides an opportunity to better integrate health considerations into coastal adaptation planning. Going forward, it will be important to ensure that protecting public health is a central goal of these assessments, alongside reducing physical and economic damage. In practice, this could include reviewing coastal protection investments to ensure that hospitals and other health infrastructure in low-lying areas are adequately protected. It may also involve strengthening water and sanitation systems in flood-prone cities to reduce disease risks, improving land-use planning to avoid new development in areas vulnerable to future flooding, and expanding mental health support for communities affected by repeated flooding or displacement.
- Redirecting Fossil Fuel Subsidies Toward Health and Clean Energy
Japan’s $70.27 billion in annual fossil fuel subsidies represents a major opportunity for policy change. Redirecting even part of this funding could support investments that protect both public health and the climate. Gradually redirecting fossil fuel subsidies toward clean energy development, climate adaptation infrastructure, and stronger healthcare systems could deliver significant benefits. Investments in renewable energy, heat adaptation measures, and workforce capacity in the health sector would not only reduce emissions but also strengthen public health resilience. Evidence from other countries suggests that clean energy investment can also generate new jobs, technological innovation, and long-term economic growth.
- Diet as a Health and Climate Opportunity
Diet is one area where climate policy and public health goals strongly overlap, but it often receives less policy attention than other sectors. The challenge now is to build on the progress already made and accelerate the shift toward more plant-rich diets that benefit both health and the environment. Several policy approaches could help support this transition. These include updating national dietary guidelines to better reflect both health and environmental considerations, incorporating plant-rich meals into public food programs such as school lunches and hospital meals, improving labeling to help consumers understand the health and environmental impact of food choices, and supporting farmers as agricultural production evolves. These types of dietary changes can deliver multiple benefits at once: reducing greenhouse gas emissions, preventing chronic diseases, and easing pressure on land and water resources. In a country facing an aging population and rising healthcare costs, promoting healthier and more sustainable diets could play an important role in improving both public health and environmental sustainability.
Conclusion: A Call to Action for 2027
The 2025 Lancet Countdown Global Report sends a clear message. Climate change is already harming human health, and the risks are growing rapidly. If global emissions continue on their current path, the world could face around 2.7°C of warming by 2100, with severe consequences for health systems, economies, and societies. At the same time, the report emphasizes that action is still possible. Rapid reductions in fossil fuel use, combined with stronger investments in climate adaptation and public health systems, can significantly reduce these risks and protect population health.
We must follow the evidence presented by the Lancet Countdown, and support policies that place human health at the center of climate action and recognize the close connection between human wellbeing and the health of the natural systems on which it depends. The path forward requires that we stop viewing climate policy as a burden on the economy and start viewing it as lifeline.
References
- Cann, K. F., Thomas, D. R., Salmon, R. L., Wyn-Jones, A. P., & Kay, D. (2012). Extreme water-related weather events and waterborne disease. Epidemiology and Infection, 141(4), 671–686. https://doi.org/10.1017/s0950268812001653
- (2022). Climate Change 2022: Impacts, Adaptation and Vulnerability. Cambridge University Press. https://www.ipcc.ch/report/ar6/wg2/
- Lancet Countdown. (n.d.). About Us. https://lancetcountdown.org/
- Lancet Countdown. (2025a). Japan Data Sheet 2025. https://lancetcountdown.org/wp-content/uploads/2025/10/Japan_Lancet-Countdown_2025_Data-Sheet.pdf
- Lancet Countdown. (2025b). The 2025 Report of the Lancet Countdown on Health and Climate Change: Summary for Policymakers. https://lancetcountdown.org/wp-content/uploads/2025/11/Policy-summary_final.pdf
- Ministry of the Environment Government of Japan. (2018). Climate Change Adaptation Act. https://www.env.go.jp/en/earth/cc/adaptation.html
- Ministry of the Environment Government of Japan. (n.d.). Special Heat Stroke Alert. https://www.wbgt.env.go.jp/en/sp/alert.php
- Ministry of Health, Labour and Welfare, Japan. (2025). STOP! Heatstroke Cool Work Campaign (Workplace Heatstroke Prevention Measures). https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000116133.html
- Romanello, M., Walawender, M., Hsu, S., et al. (2025). The 2025 report of the Lancet Countdown on health and climate change: Climate change action offers a lifeline. The Lancet, 406(10521), 2804–2857.
- Semenza, J. C., Herbst, S., Rechenburg, A., Suk, J. E., Höser, C., Schreiber, C., & Kistemann, T. (2012). Climate change impact Assessment of food- and waterborne diseases. Critical Reviews in Environmental Science and Technology, 42(8), 857–890. https://doi.org/10.1080/10643389.2010.534706
- Watts, N., Adger, W.N., Agnolucci, P., et al. (2015). Health and climate change: Policy responses to protect public health. The Lancet, 386(10006), 1861–1914.
- Willett, W., Rockström, J., Loken, B., et al. (2019). Food in the Anthropocene: The EAT-Lancet Commission on healthy diets from sustainable food systems. The Lancet, 393(10170), 447–492.
- World Health Organization. (2020). WHO guidance for climate-resilient and environmentally sustainable health care facilities. https://www.who.int/publications/i/item/9789240012226
- World Health Organization. (2025). Climate inaction is claiming millions of lives every year, warns new Lancet Countdown report. https://www.who.int/news/item/29-10-2025-climate-inaction-is-claiming-millions-of-lives-every-year–warns-new-lancet-countdown-report
- World Health Organization Regional Office for Europe. (2008). Heat-health action plans: Guidance. WHO Regional Office for Europe. https://www.who.int/publications/i/item/9789289071918
Authors
Selina Geerlings (Program Specialist, Health and Global Policy Institute)
Mako Mihira (Intern, Health and Global Policy Institute)
Eri Cahill (Associate, Health and Global Policy Institute)
Joji Sugawara (Vice President, Health and Global Policy Institute)
Top Research & Recommendations Posts
- [Research Report] Energy Conservation and Greenhouse Gas Emissions Reduction in Healthcare Facilities: Case Studies from New Construction and Facility Renewal (March 16, 2026)
- [Public Comment Submission] “The 7th Science, Technology and Innovation Basic Plan” (Draft) (February 19, 2026)
- [Research Report] Perceptions, Knowledge, Actions and Perspectives of Healthcare Organizations in Japan in Relation to Climate Change and Health: A Cross-Sectional Study (November 13, 2025)
- [Policy Recommendations] Dementia Project “The Future of Dementia Policy Surrounding Families and Others Who Care for People with Dementia” (April 27, 2026)
- [Research Report] The 2025 Public Opinion Survey on Healthcare in Japan (March 17, 2025)
- [Policy Recommendations] Mental Health Project: Recommendations on Three Issues in the Area of Mental Health (July 4, 2025)
- [Research Report] A Nationwide Survey on Cancer in Japan: 20 Years Since the Enactment of the Cancer Control Act (April 28, 2026)
- [Research Report] The 2026 Public Opinion Survey on Healthcare in Japan (February 13, 2026)
- [Policy Recommendations] Developing a National Health and Climate Strategy for Japan (June 26, 2024)
- [Announcement] Signs Health Policy Recommendations to the G7 by the C7 Global Health Working Group (March 30, 2026)
Featured Posts
-
2026-05-13
[Registration Open] HGPI Salon 2025-2026 Looking Ahead to the Future of Japan’s Social Security System “Session 5: The Value of Healthcare in Society – Perspectives from the Reiwa Era” (June 29, 2026)
![[Registration Open] HGPI Salon 2025-2026 Looking Ahead to the Future of Japan’s Social Security System “Session 5: The Value of Healthcare in Society – Perspectives from the Reiwa Era” (June 29, 2026)](https://hgpi.org/en/wp-content/uploads/sites/2/5thHGPISalon_20260629.png)
-
2026-05-15
[Registration Open] (Webinar) The 2nd J-PEP Seminar – A New Framework for Providing Information on Clinical Trial Participant Recruitment – Legal Points to Consider from the Perspective of Meaningful Involvement (June 15, 2026)
![[Registration Open] (Webinar) The 2nd J-PEP Seminar – A New Framework for Providing Information on Clinical Trial Participant Recruitment – Legal Points to Consider from the Perspective of Meaningful Involvement (June 15, 2026)](https://hgpi.org/en/wp-content/uploads/sites/2/HGPI_20260615_The2nd-J-PEPseminar.jpg)
-
2026-05-18
[Registration Open] Kick-off Panel Discussion “From Japan and Africa, in Discussion with the World: Cultivating Together a Philosophical Dialogue on Health” (June 15, 2026)
![[Registration Open] Kick-off Panel Discussion “From Japan and Africa, in Discussion with the World: Cultivating Together a Philosophical Dialogue on Health” (June 15, 2026)](https://hgpi.org/en/wp-content/uploads/sites/2/HGPI_20260615_Eyecathch_panel-discussion-From-Japan-and-Africa-in-Discussion-with-the-World‗02.png)
-
2026-05-19
[Registration Open] (Webinar) HGPI Special Seminar “Building a Society Where People Live with Blood Disorders: The Future of Blood Disorder Policy as Examined from the Frontlines of Home-Based Care × Lived Experience Research” (June 12, 2026)
![[Registration Open] (Webinar) HGPI Special Seminar “Building a Society Where People Live with Blood Disorders: The Future of Blood Disorder Policy as Examined from the Frontlines of Home-Based Care × Lived Experience Research” (June 12, 2026)](https://hgpi.org/en/wp-content/uploads/sites/2/HGPI_20260515_HGPI-Special-Seminar-Blood-Disorders.png)












